Clinical Review
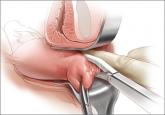
2015 Update on vaginal hysterectomy
A few innovative tools can greatly ease the operative experience for both surgeon and patient

An expert vaginal surgeon details her technique for this procedure, including tips and tricks to facilitate surgery in a woman with a narrow introitus
In this Article
In the United States, gynecologic surgeons remove approximately one uterus every minute of the year.1 That rate translates to more than 525,000 hysterectomies annually in this country alone. Yet, despite the widespread availability of information on the benefits of a vaginal approach to hysterectomy, the great majority of these operations—close to 50%—are still performed via an open abdominal approach.2
As I pointed out last month in my “Update on Vaginal Hysterectomy,” the vaginal approach not only is more cosmetically pleasing than laparoscopic and robot-assisted hysterectomy (not to mention open abdominal surgery) but also has a lower complication rate.3
As I also noted, one reason for the low rate of vaginal hysterectomy may be the assumption, on the part of many gynecologic surgeons, that the techniques and tools they learned to use during training are still the only options available today. That assumption is wrong.
In this article, I describe the technique for vaginal hysterectomy using basic instru mentation. This article is based on a master class in vaginal hysterectomy produced by the AAGL and co-sponsored by the Am erican College of Obstetricians and Gynecologists and the Society of Gynecologic Surgeons. This master class offers continuing medical education credits and is avail able at http://www.aagl.org/vaghystwebinar.
For a look at innovative tools for this procedure, see my “Update on Vaginal Hysterectomy” in the September 2015 issue of this journal at obgmanagement.com.
Vaginal hysterectomy has few contraindications
Many commonly cited contraindications to the vaginal approach are not, in fact, absolute contraindications. An open or laparoscopic approach is preferred when the patient has a known cancer, of course, and when deep infiltrating endometriosis is present at the rectovaginal septum. However, previous pelvic surgery, nulliparity, an enlarged uterus, or lack of a prior vaginal delivery need not exclude the vaginal approach. Nor does a narrow introitus necessarily mandate a laparoscopic or open abdominal approach. In fact, in this article, I describe my basic technique in a patient (a cadaver) with a very narrow pubic arch, and I offer strategies for gaining some needed mobility and avoiding complications (TABLES 1 and 2).
TABLE 1. 5 solutions to difficult vaginal access |
• Be flexible in your choice of retractors. • Eliminate as much metal as possible; a retractor may not always be necessary. • Maintain a detailed knowledge of anatomy—and know it upside down! • Carry out careful dissection and clamp placement prior to peritoneal entry anteriorly or posteriorly. • Split the cervix carefully in the midline to delineate the bladder reflection. |
| TABLE 2. Avoiding complications: 7 pearls |
• Position the patient carefully, with the buttocks at least 1 inch over the edge of the table, and pad the sacrum on thin patients. • Use routine prophylaxis for deep venous thrombosis (DVT). • Give 1 dose of a 1st-generation cephalosporin approximately 15 to 30 minutes prior to the initial incision. • Maintain meticulous hemostasis. • Handle all tissue carefully, as though the patient were awake. • Ensure early ambulation to reduce the risk of DVT. • Avoid use of an indwelling catheter. |
Next month, in the November issue of OBG Management, John B. Gebhart, MD, will describe his vaginal technique for right salpingectomy with ovarian preservation, as well as his technique for right salpingo-oophorectomy.
Proper patient positioning is key
You can simplify the operation by positioning the patient so that her buttocks are over the edge of the table fairly far—at least 1 inch beyond the edge of the table for optimal exposure and greater access. If the patient is thin, it then becomes important to pad the sacrum because, when she is positioned that far off the table, all her weight comes to rest on the sacrum. In overweight patients, this is not an issue, but for thin patients, I place a bit of egg crate or gel beneath the sacrum.
For the procedure, I prefer to place my instruments on a tray that is kept on my lap. This arrangement frees the scrub technician from having to hand tools over my shoulder—and it saves time. I use a narrow, covered Mayo stand, and I place a stepstool beneath my feet to keep my knees at right angles so that things don’t slip during the operation.
Surgical technique
Choose an appropriate retractor
In a woman with a narrow introitus, I find that a posterior weighted speculum takes up too much space. Once I place a clamp on the cervix with that speculum in place, I don’t have much room to work. However, if I substitute a small Deaver retractor, which is narrower, I gain more workspace.

A few innovative tools can greatly ease the operative experience for both surgeon and patient
Vaginal hysterectomy is a 21st Century approach, thanks to tools, techniques, and other refinements from the fields of laparoscopy and robotics
Sacrospinous hysteropexy and vaginal hysterectomy with uterosacral ligament suspension were found to be comparable at 12 months after surgery in...
