Chest Infections
Antibiotics that "mist the target"
The increase in multi-drug resistance (MDR) and the dearth of new antibiotics in the "pipeline" has prompted interest in aerosolized antibiotics (AA) for treating ventilator-associated pneumonia (VAP). Toxic antibiotics like colistin may be aerosolized, reaching high concentrations in distal airways with minimal systemic absorption.
Aerosolized antibiotics have mostly gained traction in the "adjunctive" role (added to systemic antibiotics). Advances in nebulizer technology, and adjustments in ventilator settings and the breathing circuit to optimize drug delivery, have paved the way for clinical application.
Rattanaumpawan and colleagues randomized 100 patients with VAP due to MDR gram-negative bacilli (GNB) to aerosolized colistin vs placebo in addition to IV antibiotics, without benefit in clinical outcomes (J Antimicrob Chemother. 2010;65[12]: 2645).
Three recent studies used advanced vibrating plate aerosolization: Lu and colleagues compared aerosolized colistin +/- IV aminoglycoside in 43 patients with VAP with MDR GNB vs IV antibiotics alone in 122 others with sensitive GNB (Anesthesiology. 2012;117[6]:1335); outcomes were similar.
In another study, 40 patients with drug-susceptible GNB received inhaled-only ceftazidime plus amikacin, vs systemic antibiotics. Treatment success was nonsignificantly higher in the aerosol-only group; antibiotic resistance developed only in the IV group (Am J Respir Crit Care Med. 2011;184[1]: 106). Niederman and colleagues, in a randomized VAP trial (n=69), found adjunctive inhaled amikacin reduced overall exposure to antibiotics with less clinical failure compared with control (Intensive Care Med. 2012;38[2]:263).
The advantage of AA may be in avoiding systemic antibiotic overexposure. Further studies will investigate adjunctive vs stand-alone AA, optimal dosing strategies, and agents for gram-positives.
Dr. Paul Richman, FCCP
Steering Committee Member
Dr. Michael Niederman, FCCP
Chair
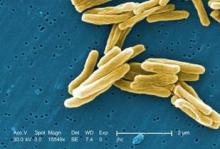 Photo Credit: Janice Carr, Centers for Disease Control and Prevention
Photo Credit: Janice Carr, Centers for Disease Control and Prevention
Tuberculosis: Human trials and decades of clinical experience with bacillus Calmette-Guerin have shown that it is useful for prevention of TB, and particularly for interdiction of major complications of TB (dissemination, meningitis, and mortality) in children.
BCG vaccination for TB: Time for a reexamination?
Bacillus Calmette-Guerin (BCG) is the single most widely used human vaccine in history, with over 3 billion individuals vaccinated in total and 100 million annually(Liu et al. Hum Vaccine. 2009;5[2]:70).
The vaccine was developed in the early 20th century from a strain of Mycobacterium bovis. The original virulent strain had become attenuated by numerous subcultures in vitro over 13 years by Calmette and Guerin(McShane et al. Tuberculosis [Edinb]. 2012;92[3]:283).
Over the past 100 years, BCG has been disseminated to many laboratories and countries for use and has required frequent subculturing. As a result, the strains have diverged and do not have the same virulence properties as the original, and BCG should not be viewed as a single organism(Liu et al. Hum Vaccine. 2009;5[2]:70). Strain divergence has been reduced due to lyophilization of cultures over the past 47 years. Naturally occurring mutants of BCG have deletions of major virulence factors that affect the ESX-1 protein secretion system, one of several secretion systems found in the TB genome. Absence of these proteins results in impaired growth of TB in macrophages, modulates phagolysosomal fusion, and reduces bacterial virulence. The ESX-1 secretion system plays a major role in virulence of TB, and loss of the system accounts for much of the loss of virulence of BCG (Liu et al. Hum Vaccine. 2009;5[2]:70). These mutations may contribute to differences in side effects and efficacy of the vaccine utilized in different locales.
Other virulence factors of TB and BCG relate to the lipid content/composition of the cell wall of mycobacteria. These lipids are also integrally involved in pathogenicity(Liu et al. Hum Vaccine. 2009;5[2]:70). Absence or mutations in these lipids result in attenuation of infection in both mouse and guinea pig models.
Human trials and decades of clinical experience with BCG have shown that it is useful for prevention of TB and particularly for interdiction of major complications of TB (dissemination, meningitis, and mortality) in children(Checkley et al. Trends Pharmacol Sciences. 2011;32[10]:601; Trunz et al. Lancet. 2006;367[9517]:1173).
The responses for pulmonary TB in younger and older adults are not as robust (Colditz et al. JAMA. 1994;271[9]:698). For decades, the World Health Organization (WHO) has recommended BCG in high-risk endemic areas and for children. BCG is not recommended in general in developed countries where the endemic rate of TB is low; the utility of the skin test for diagnosis of latent TB would be compromised and the false-positivity rate of the test would be high.
Recognizing that BCG is not an ideal vaccine despite its widespread utility and experience over decades, further research has used the results of BCG attenuation to pursue avenues to improve BCG or to advance other vaccine candidates(Liu et al. Hum Vaccine. 2009;5[2]:70; McShane et al. Tuberculosis [Edinb]. 2012;92[3]: 283; Checkley et al. Trends Pharmacol Sciences. 2011;32[10]:601; Jeyanathan et al. J Immunol. 2008;181[8]:5618; Hokey et al. Tuberculosis [Edinb]. 2011;91[1]:82; Morais et al. Tuberculosis [Edinb]. 2010;90[2]:135; McShane et al. Philos Trans R Soc Lond B Biol Sci. 2011;366[1579]:2782; Rowland et al. Expert Rev Vaccines.2011;10[5]:645).

